Incretin Effect GLP-1 Therapy: A Revolutionary Approach to Managing Type 2 Diabetes
The Incretin Effect: A Key to Understanding GLP-1 Therapy
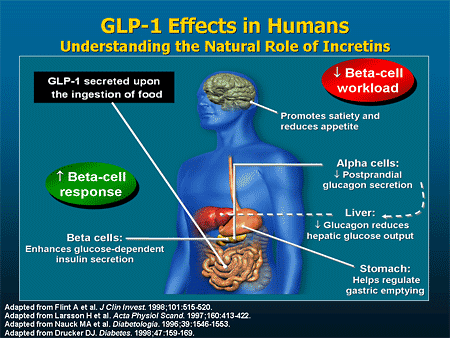
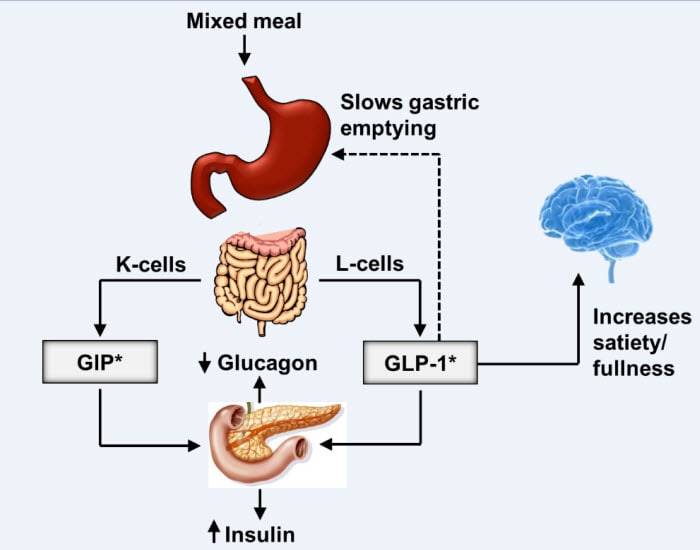
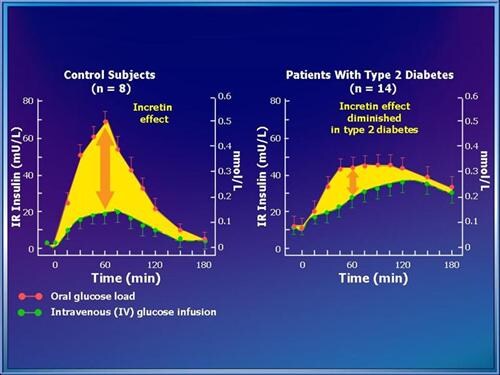
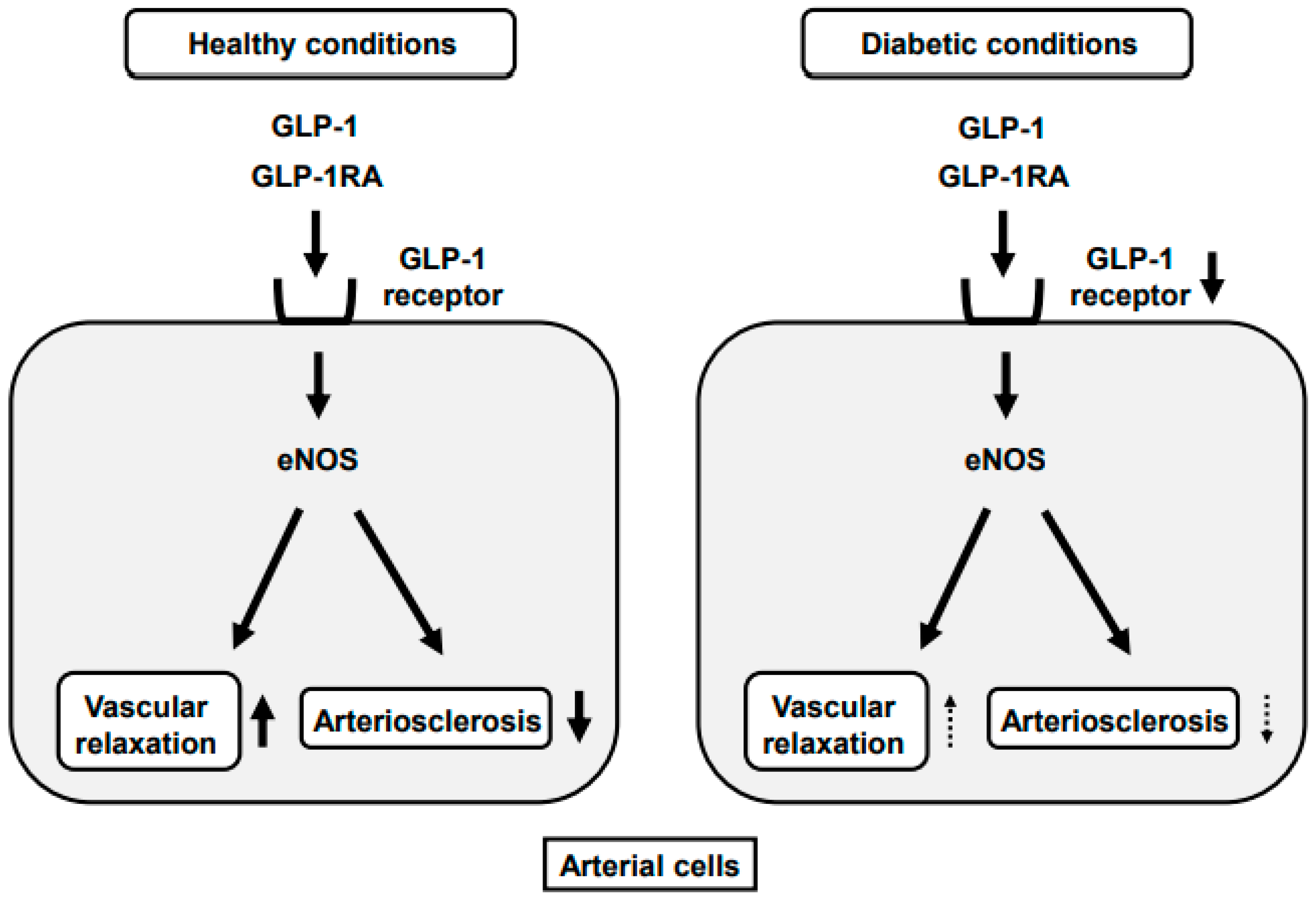
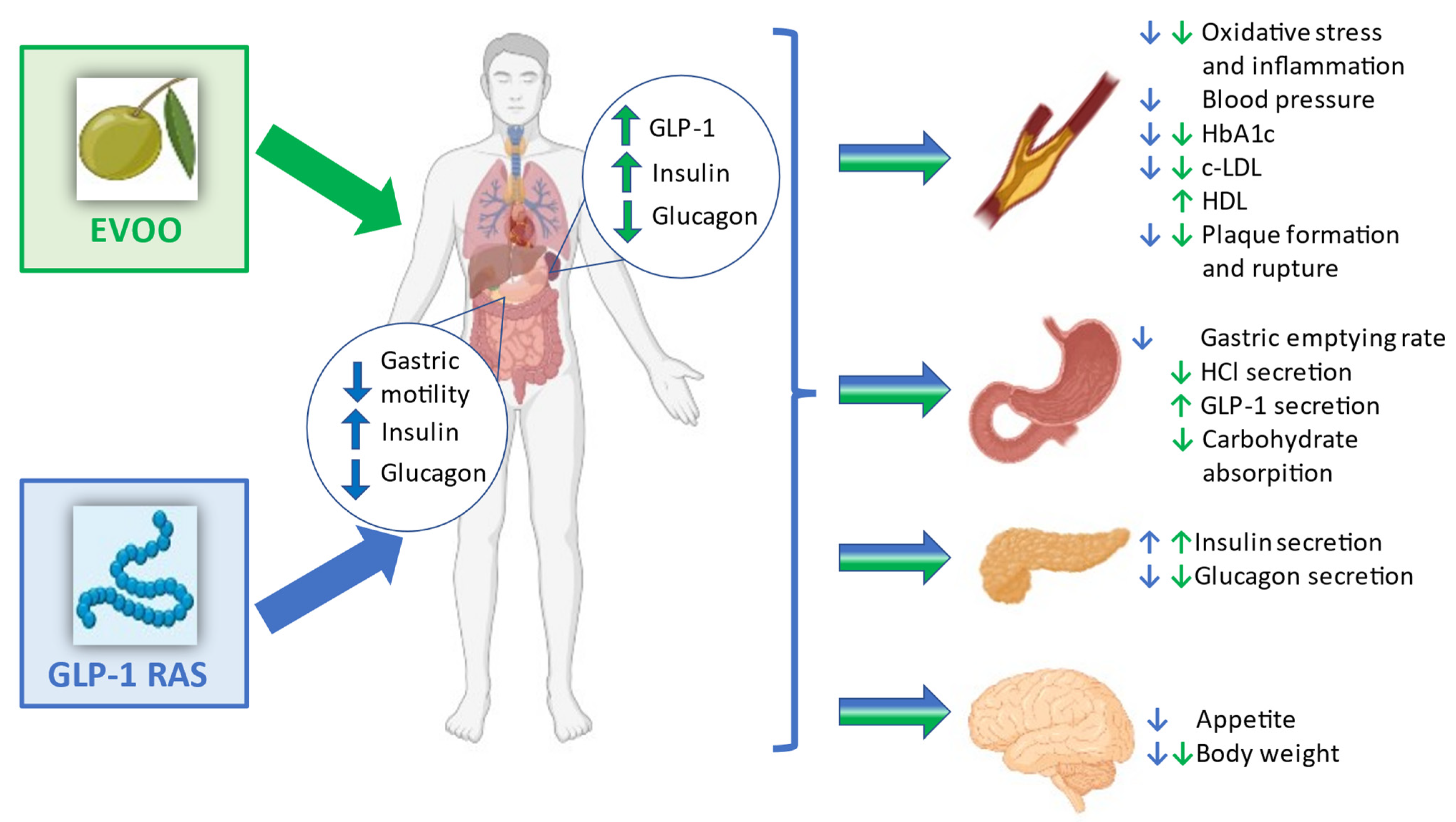
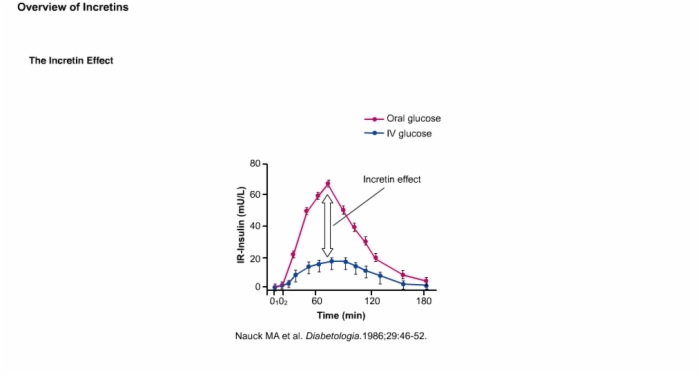
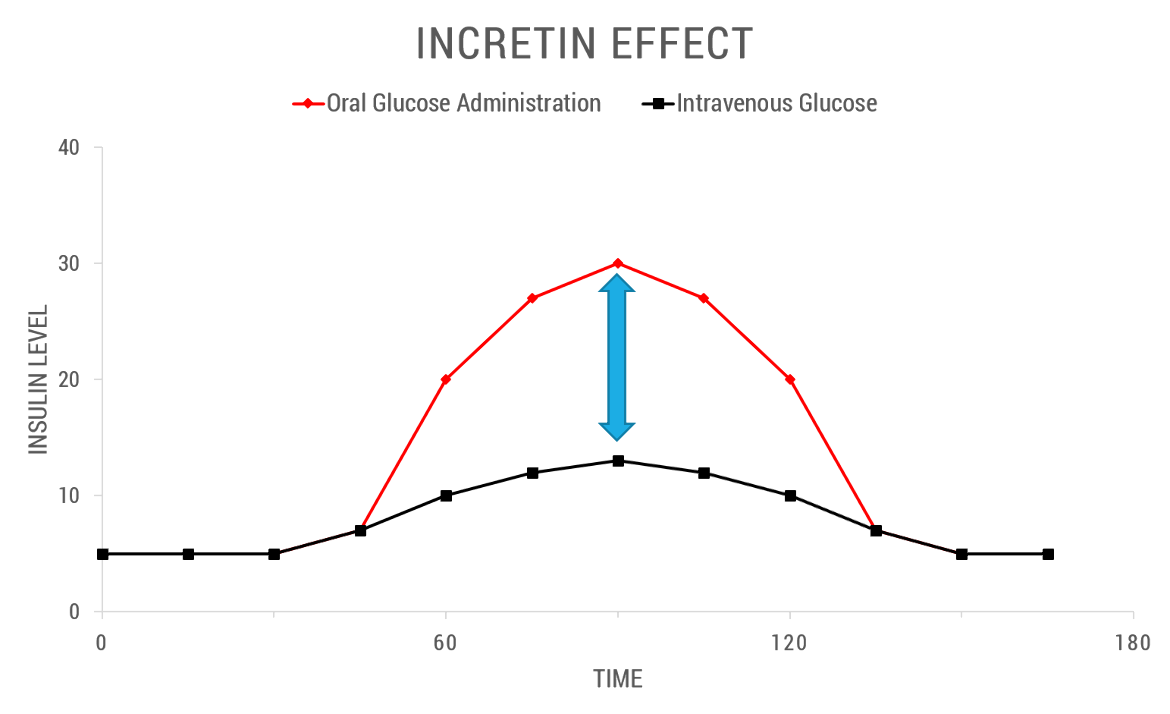
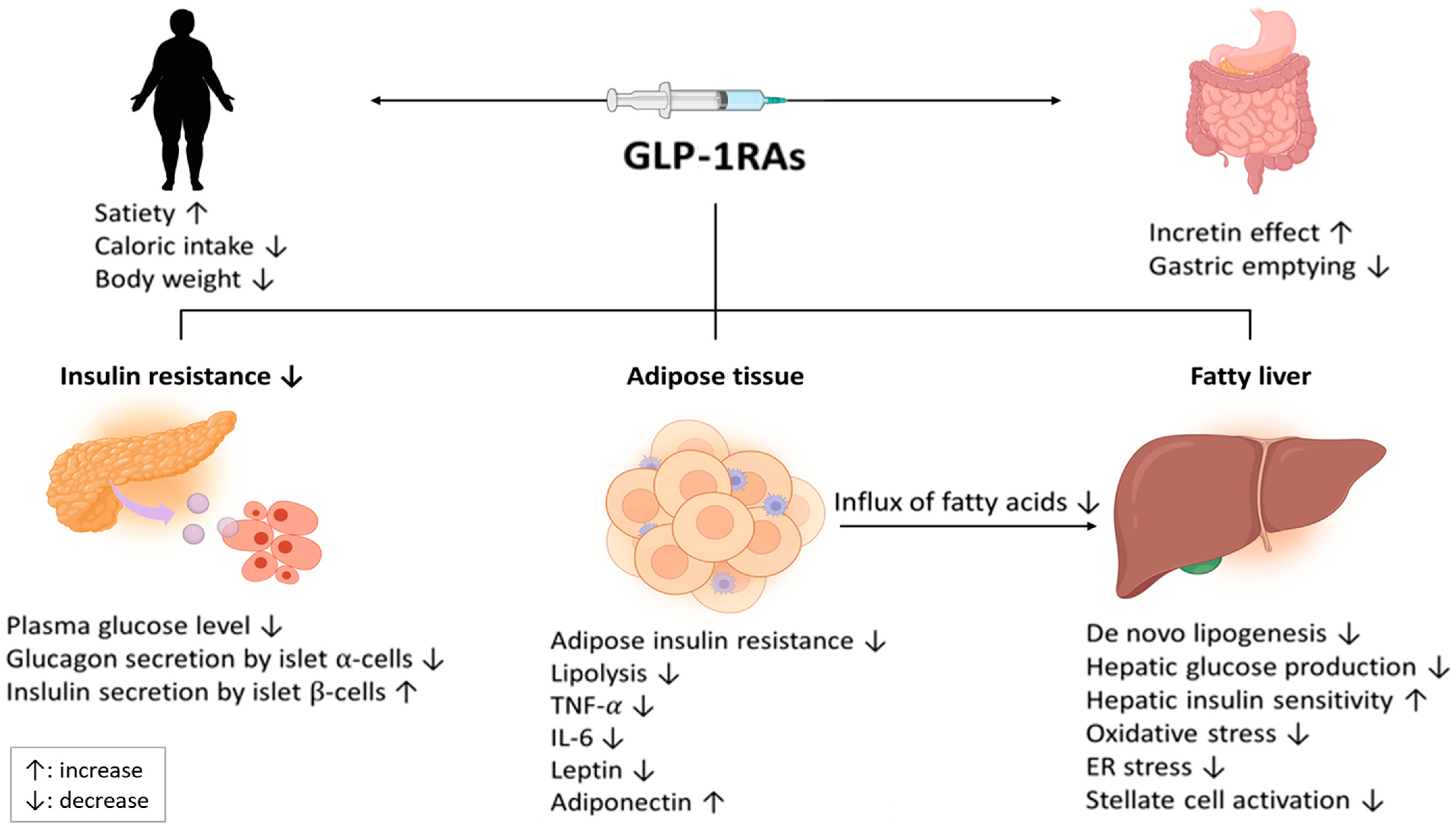
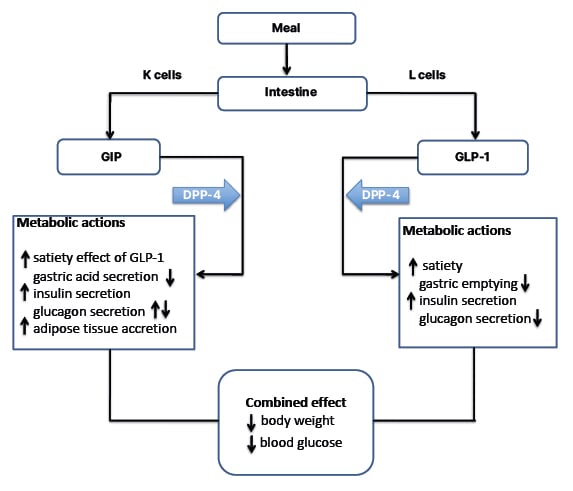
The incretin effect refers to the augmented insulin secretion in response to nutrient intake, which is partly attributed to the release of intestinal hormones such as GLP-1. GLP-1 plays a crucial role in regulating blood sugar levels by stimulating insulin release, inhibiting glucagon secretion, and slowing gastric emptying. In type 2 diabetes, the incretin effect is impaired, leading to inadequate insulin secretion and hyperglycemia.
How GLP-1 Receptor Agonists Work
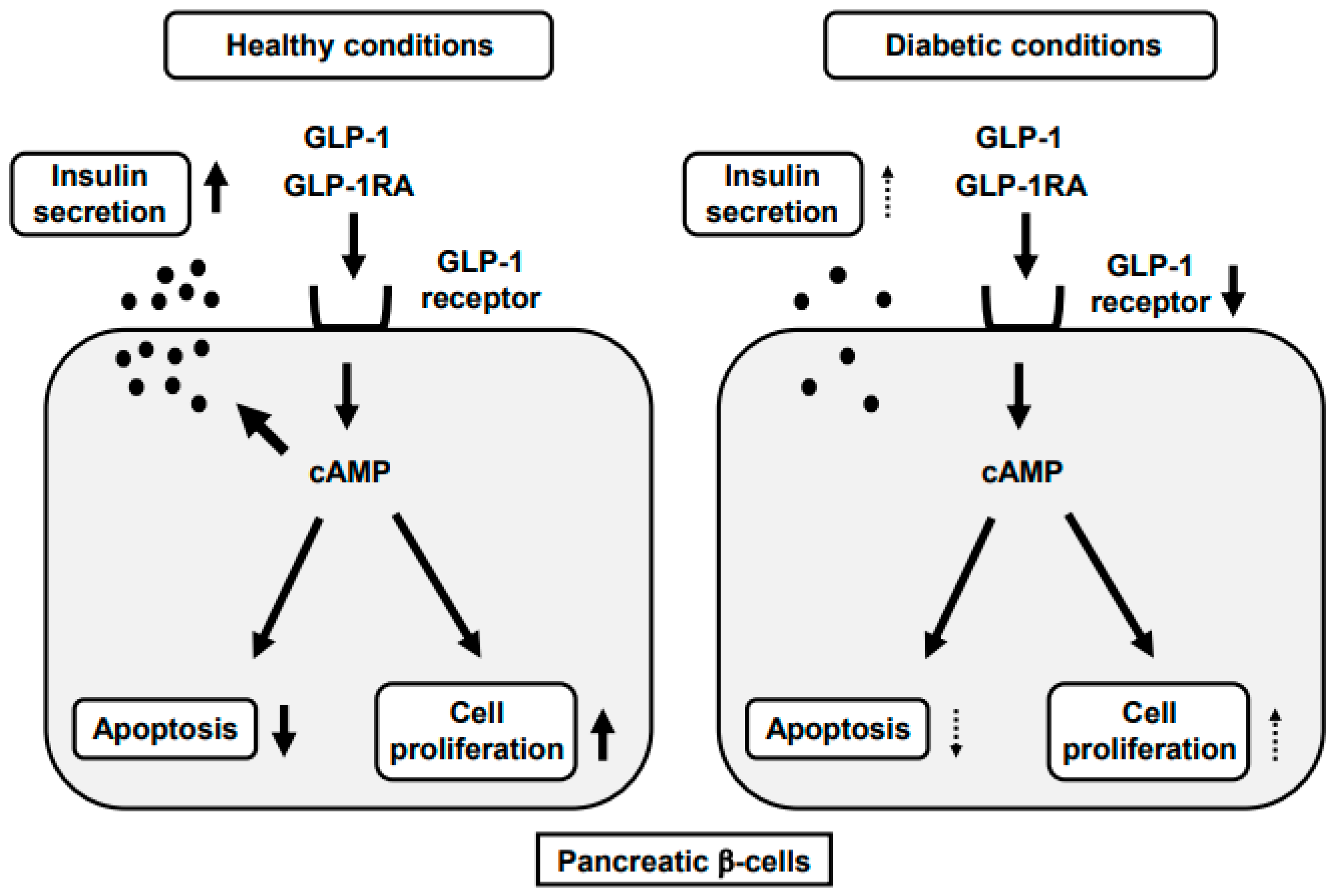
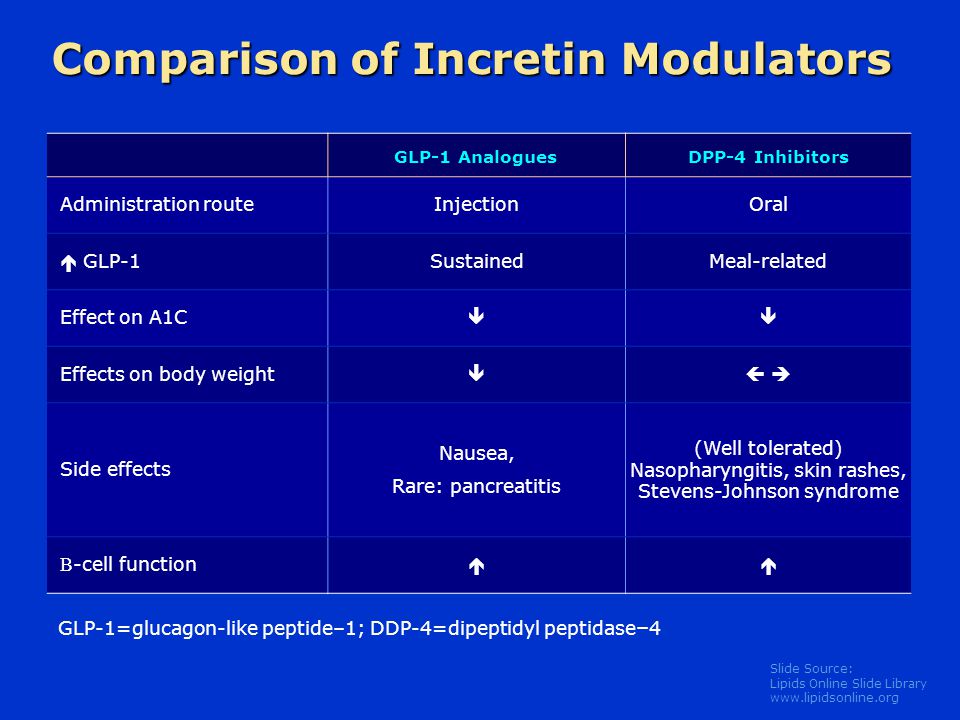
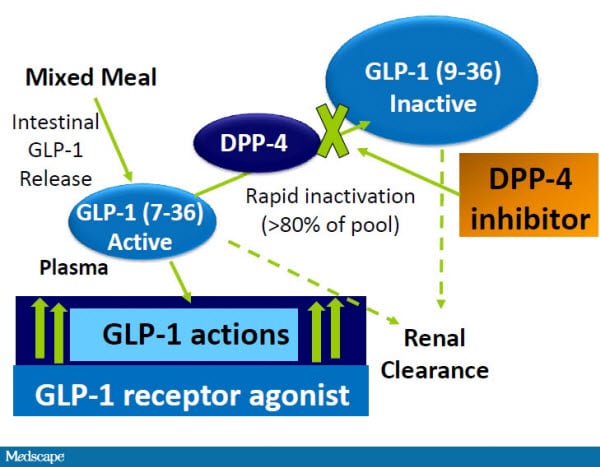
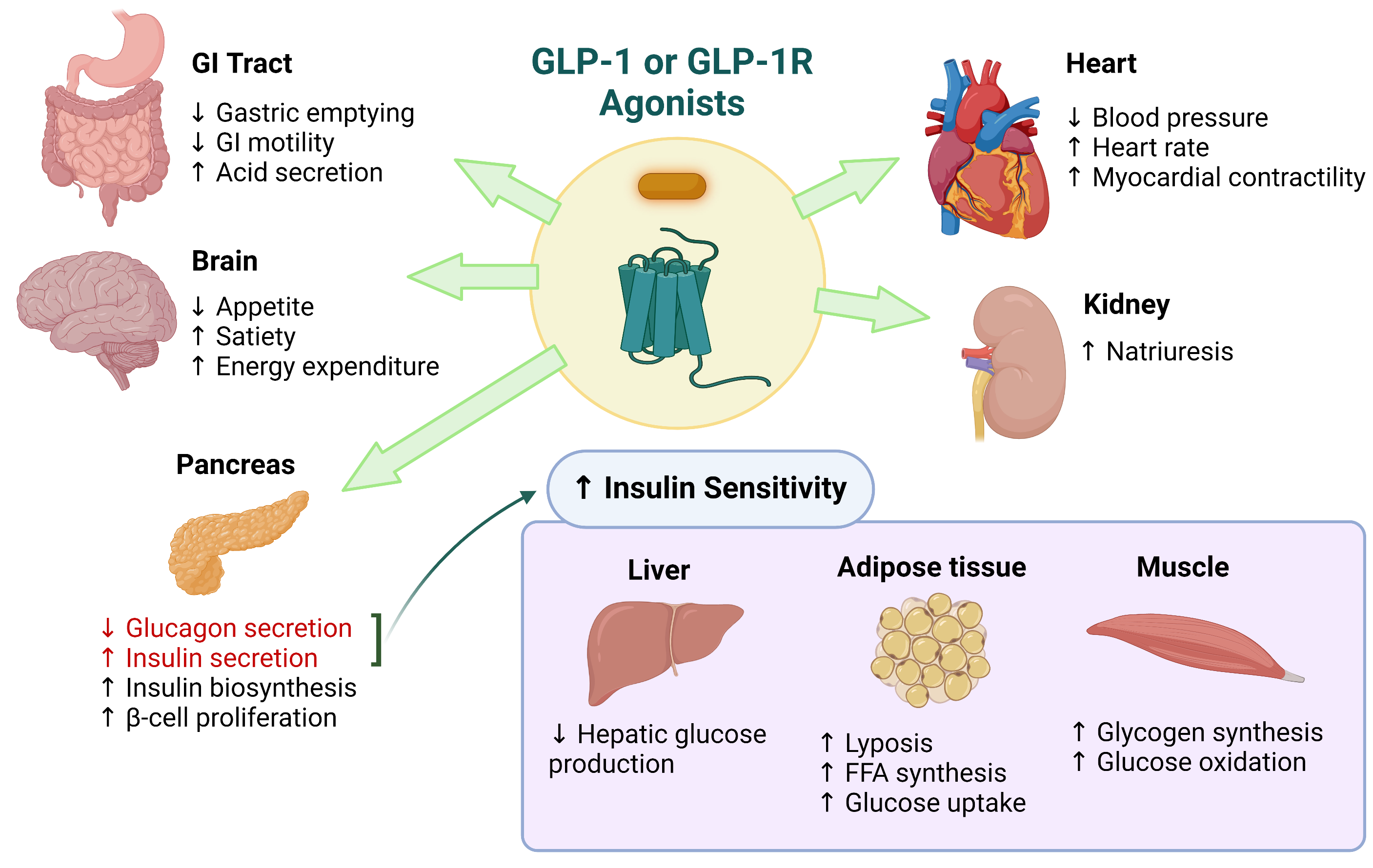
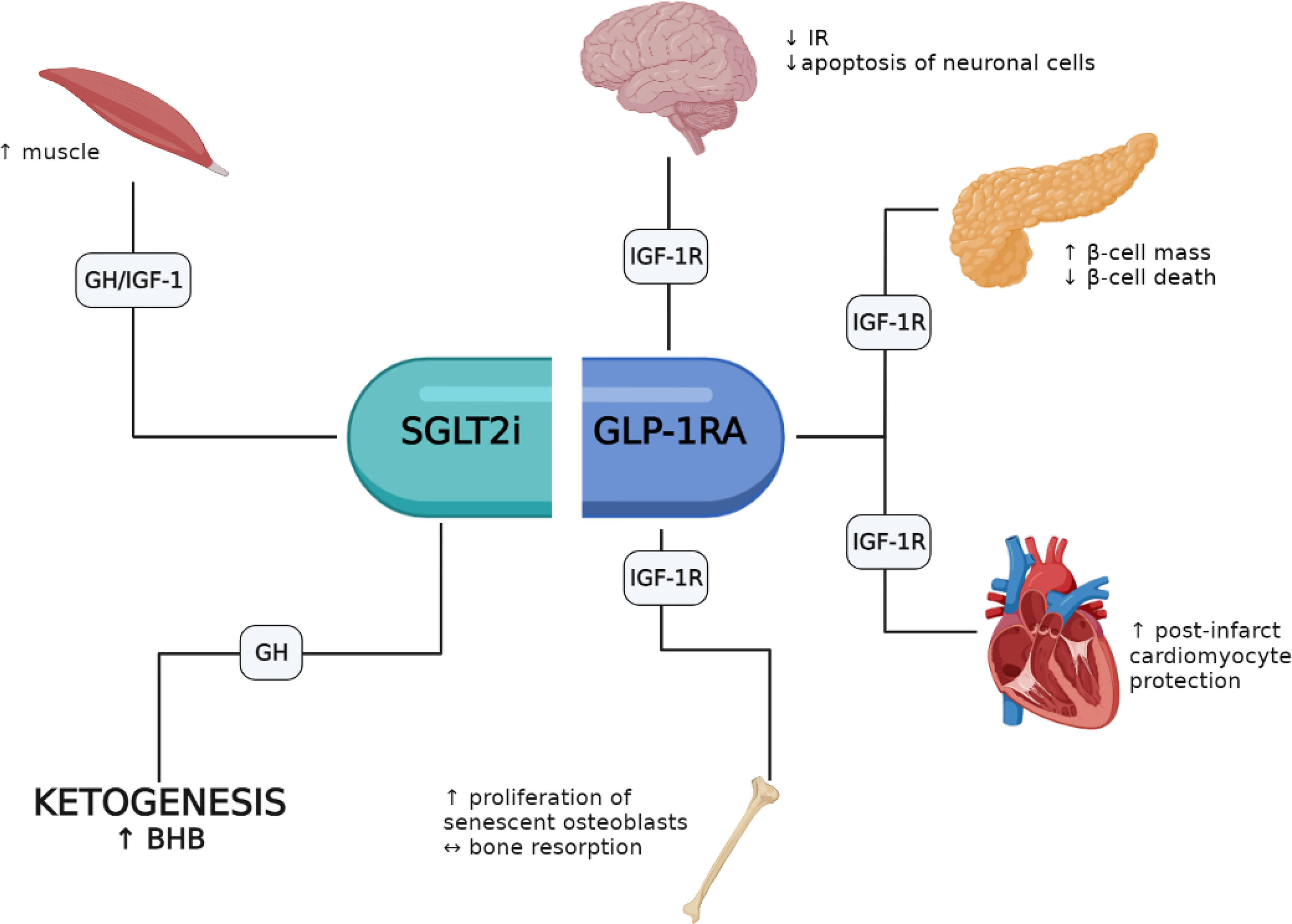
GLP-1 receptor agonists, such as exenatide and liraglutide, mimic the actions of endogenous GLP-1 by binding to its receptor on pancreatic β-cells. This binding stimulates insulin release, suppresses glucagon secretion, and slows gastric emptying, resulting in improved glycemic control and weight reduction. GLP-1 agonists also have a low risk of causing hypoglycemia, making them an attractive option for patients with type 2 diabetes.
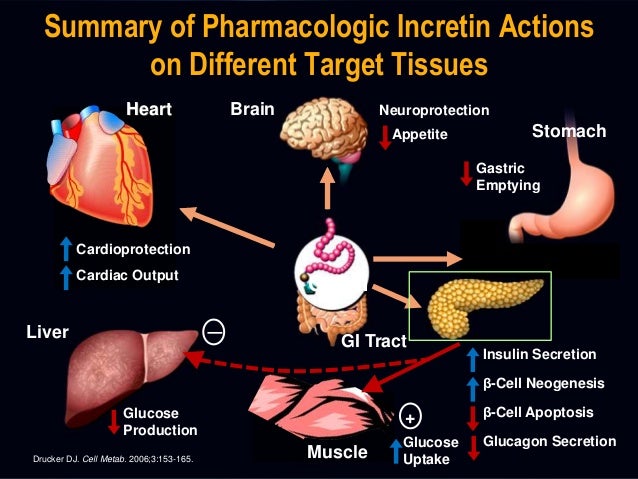
As we can see from the illustration, Incretin Effect Glp-1 Therapy has many fascinating aspects to explore.
Benefits of GLP-1 Therapy
- Improved glycemic control: GLP-1 agonists have been shown to reduce HbA1c levels and improve fasting plasma glucose levels.
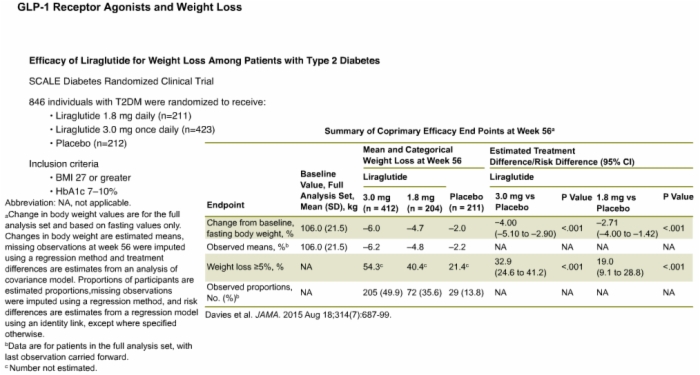
- Weight reduction: GLP-1 agonists can lead to significant weight loss, often exceeding 5% of initial body weight.
- Low risk of hypoglycemia: GLP-1 agonists have a low risk of causing hypoglycemia, making them a safer option for patients with type 2 diabetes.
- Cardiovascular benefits: Some GLP-1 agonists, such as semaglutide, have been shown to reduce major adverse cardiovascular events (MACE) and cardiovascular mortality.
Potential Side Effects of GLP-1 Therapy
- Nausea and vomiting: GLP-1 agonists can cause nausea and vomiting, especially during the initial treatment period.
- Diarrhea: GLP-1 agonists can lead to diarrhea, which may be a result of slowed gastric emptying.
- Injection site reactions: Some patients may experience injection site reactions, such as redness, swelling, or itching.
- Increased risk of pancreatitis: GLP-1 agonists have been associated with an increased risk of pancreatitis, although the exact mechanism is unclear.
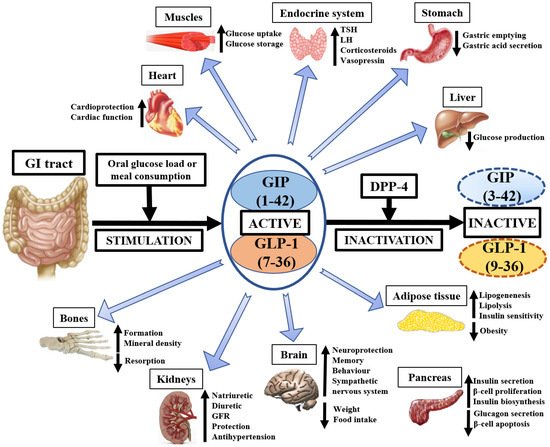
Moving forward, it's essential to keep these visual contexts in mind when discussing Incretin Effect Glp-1 Therapy.
GLP-1 therapy represents a significant advancement in the treatment of type 2 diabetes, offering a unique combination of glycemic control, weight reduction, and a low risk of hypoglycemia. While GLP-1 agonists have a favorable safety profile, potential side effects such as nausea, diarrhea, and injection site reactions should be monitored. As research continues to uncover the intricacies of the incretin effect and GLP-1 therapy, we can expect even more innovative treatments to emerge, revolutionizing the management of type 2 diabetes.
Future Directions
With the increasing understanding of the incretin effect and GLP-1 therapy, researchers are exploring new avenues for treatment, including:
- Dual GLP-1 and GIP agonists: These agents target both GLP-1 and glucose-dependent insulinotropic polypeptide (GIP) receptors, potentially offering enhanced glycemic control and weight reduction.
- Triple GLP-1, GIP, and glucagon agonists: These agents simultaneously target GLP-1, GIP, and glucagon receptors, which may lead to improved energy expenditure and glycemic control.
- Oral GLP-1 agonists: Researchers are working on developing oral GLP-1 agonists, which could potentially offer a more convenient treatment option for patients.

This particular example perfectly highlights why Incretin Effect Glp-1 Therapy is so captivating.
References
This article is based on the following sources:
- Ignatova E, et al. (2020). GLP-1 receptor agonists: A review of their mechanism of action, efficacy, and safety. Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy, 13, 2727–2742.
- Drucker DJ, et al. (2020). GLP-1 receptor agonists: A review of their clinical efficacy and safety in type 2 diabetes. Diabetes, Obesity and Metabolism, 22(3), 553–565.
- Nauck MA, et al. (2020). GLP-1 receptor agonists: A review of their pharmacology, pharmacokinetics, and clinical use. Diabetes, Metabolic Syndrome and Obesity: Targets and Therapy, 13, 2711–2726.
Conclusion
In conclusion, GLP-1 therapy represents a revolutionary approach to managing type 2 diabetes, offering improved glycemic control, weight reduction, and a low risk of hypoglycemia. As research continues to uncover the intricacies of the incretin effect and GLP-1 therapy, we can expect even more innovative treatments to emerge, transforming the management of type 2 diabetes.